The treatment process
In the Radiosurgery Center in Debrecen,
recently, new sources have been installed in the
treatment device. With these treatments
usually take between 20-40 minutes. This can
vary depending on the type and size of the
lesion, in some cases, can be up to 1.5-2 hours.
The procedure involves preparations that
require a one-night hospital stay, and after the
treatment, the patient can only be discharged
with an escort.
Accommodation is available for
the escorts at the clinic or in the city and the
cost involved are agreed with everyone
beforehand. If the patient has a valid health
insurance, the travel costs may be reimbursed.

The day before treatment: a new MR scan is needed for accurate targeting
The day before the treatment, the patient is
admitted to the Neurosurgery Department,
where an MRI scan is taken. It is required for
the preparation for planning the radiosurgical
procedure.
A combined MRI-CT image is generated with
the use of a contrast-enhanced CT scan on the
day of the treatment to image the lesions in as
much detail as possible. The combined image is
used to define the spherical target irradiation
areas of the treatment.
The patient needs to spend the night at the
hospital, so that preparations can begin early in
the morning on the day of the treatment.
Preparation: frame attachment to ensure secure positioning of the head
Early in the morning on the day of the
treatment, the nurse specialist of the Gamma
Radiosurgery Center places a cannula in the
arm of the patient for the contrast-enhanced
CT scan.
The patient is only allowed to drink
noncarbonated water from the morning on because the treatment needs to be done on an
empty stomach.
To ensure accurate targeting, the head of the
patient is securely fixed to the treatment device
so that the gamma rays only reach
predetermined locations of the lesion.
The fixation is ensured with a stereotaxic frame,
which also serves as a 3-dimensional coordinate
system for radiation surgery planning.
The contrast-enhanced CT scan for radiation
surgery planning is already taken with the
frame attached to the head of the patient,
therefore the frame attachment is done in the
CT operator room of the Department of
Neurosurgery.
The frame is attached to the skull at four points,
on two sides of the back of the head and two
sides of the forehead. A local anesthetic is
applied before the application of the fixation
screws through the skin. After the frame is
attached, a feeling of tightness might occur and
disappears later.
After the contrast CT scan, the patient is
transferred by a local ambulance to the Gamma
Radiosurgery Center.

Irradiation planning: the work of a team of dedicated professionals
The precision part of the procedure is the irradiation planning, which is done jointly by the neurosurgeon, the radiotherapist, and the radiation physicist. The neurosurgeon designs the course of the treatment using a dedicated computer to determine the 3-dimensional coordinates of the target area in relation to the stereotactic frame on the head of the patient. The same procedure defines the size of the target area and the radiation dose to be delivered during the treatment. The physicist confirms the coordinates and the dose rate to ensure the accuracy of the procedure. The planned dose depends on the histology of the disease, the size and location of the area to be treated, and the dose delivered in potential previous radiation treatments. Radiation planning takes about half an hour, during which time the patient is in the relaxation room with their escort.
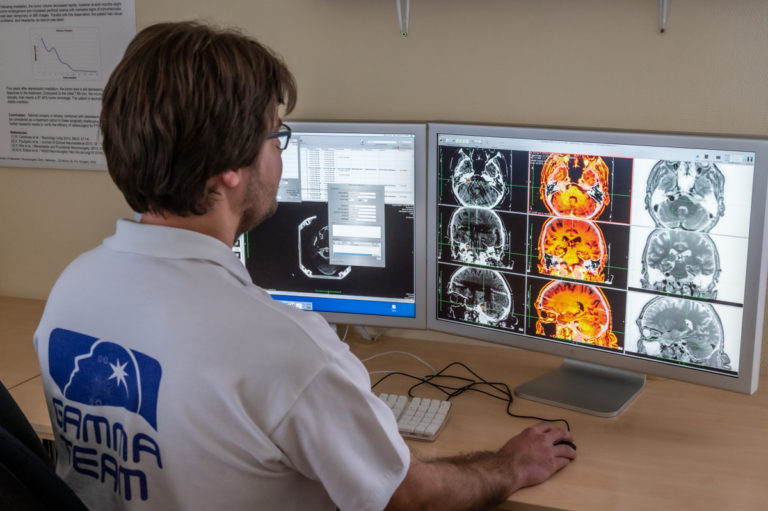
Treatment procedure: in complete safety and without pain
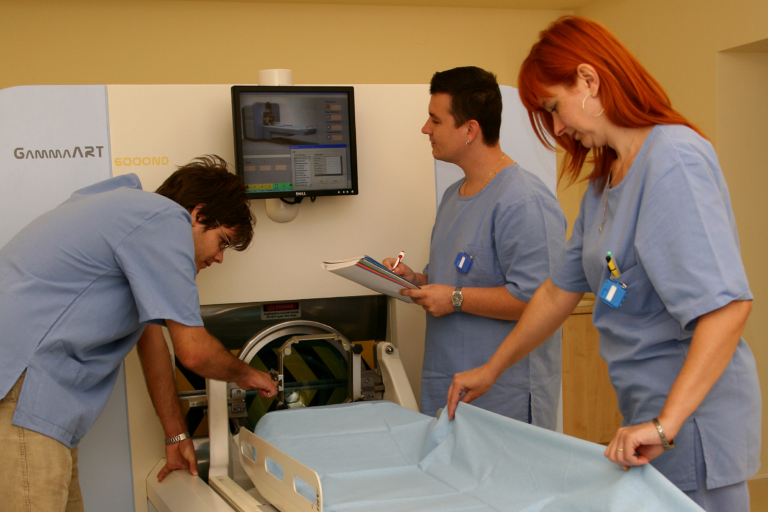
Once the planning is complete, the patient is
escorted to the air-conditioned treatment
room, where they are placed on the
radiosurgery equipment.
The rotating radiosurgery system for radiation
surgery resembles in its geometry to an MRI
machine. The frame attached to the skull of the
patient is inserted into the frame holder to
prevent the head from moving during the
treatment; and to ensure that the radiation
beams converge precisely on the target area to
initiate the process of tumor tissue necrosis.
During the treatment, the patient is alone in
the treatment room, but they are constantly
monitored by video cameras and can
communicate with the personnel via a built-in
microphone. For the the complete treatment of
the lesion, the machine might have to be
repositioned several times during the
procedure. During these times, several staff
members assist the patient to prepare for the
next phase of the procedure.
Completion of the treatment: frame removal and monitoring
At the end of the treatment, the frame is removed, and the small wounds are treated with a bandage and a covering band. The patient is provided information on the date and procedure of the follow-up diagnostic imaging. At this point, the patient is allowed to eat, and after a few hours of observation, in most cases, is discharged home the same day. For the discharge, an escort needs to be present to ensure the safety of the patient leaving the center. After a day of rest at home, the patient can resume normal activities if other existing medical conditions allow.